Alastair Campbell: I urged couples counselling for Blair and Brown
Herald Scotland:
The former Downing Street spin doctor said consulting mental health professionals would improve how they dealt with stress and make them better leaders.
Mr Campbell also revealed that he urged Tony Blair and Gordon Brown to seek couples counselling when their working relationship disintegrated in government - but the prime minister rejected the idea.
• The Independent: You don't have to seek psychiatric help if you're a politician, but why wouldn't you?
Psychotherapy provision in the UK: time to think again
A marvellous riposte to the waiting-list-then-brief-CBT model of mental heath care, from The Lancet:
If a patient with cancer had to wait up to a year for treatment, health-care professionals and the general public would think it dangerous and wrong. If their treatment was then limited to six doses of radiotherapy, regardless of the pace of recovery, there would be disbelief. And if one treatment approach did not work when alternative therapies were available, it would be scandalous for a clinician to then say “there is no more we can do for you”. Yet this is often the experience of people suffering from psychological distress trying to access therapy on the NHS.
Armed forces suffering crisis as 28,000 are diagnosed with problems since 2007
Mirror.co.uk:
More than 28,000 members of the armed services have been diagnosed with mental health problems since 2007.
The rocketing numbers sought help from Ministry of Defence services for a wide range of conditions in that time.
Charities and MPs tonight branded the figures “alarming” and demanded defence chiefs act to tackle the crisis.
Kevan Jones, Labour’s shadow armed forces minister, told the Sunday People : “This highlights the need to concentrate on military mental health and also ensure the NHS deals with service veterans.
"The rise is partly because of the wars in Afghanistan and Iraq. But it’s also because personnel are more aware of the help available and ask for diagnosis – which is a good sign.
“It’s vital to ensure there’s a joined-up connection between the military’s mental health and the NHS so when troops leave service they get vitally needed help.”
The figures, revealed after a question in Parliament last week, show that in 2014 about 5,159 troops were diagnosed with mental health problems at specialist centres – up from 3,560 in 2007.
Suicide in Wales
BBC News:
A man who says he has lost 19 friends to suicide over three decades has spoken out so that other people might think twice about killing themselves.
Filmmaker Andrew Jenkins, 52, from Blaenau Gwent, plans to make an educational film about the issue.
This comes as the latest figures show a sharp rise in suicide rates in Wales, particularly among men.
In 2013, 393 suicides were recorded in Wales, up from 334 in 2012.
The number of men taking their own lives has risen from 21.4 in 2012 to 26.1 per 100,000 population in 2013, which is the highest figure since 1981.
The rate for women in Wales is 5.8, down from 5.9 in 2012.
The Welsh rate of suicide is higher than the UK figure of 11.9 deaths in 2013.
International news
Where are the mental-health providers?
Wall Street Journal:
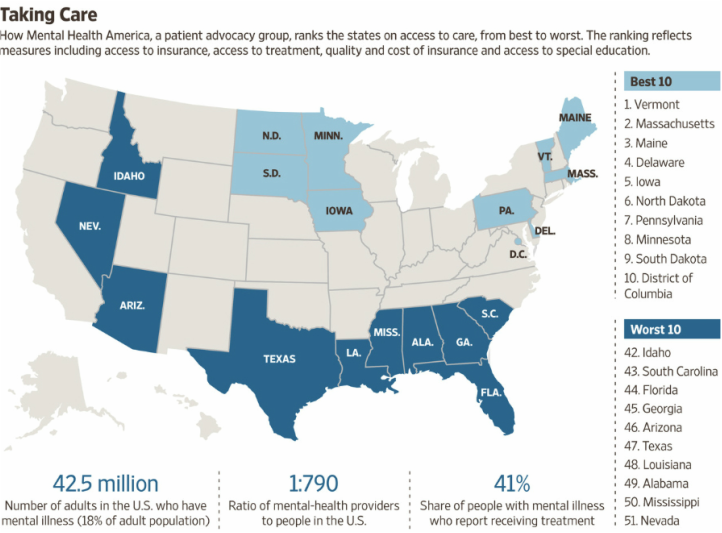
Millions of Americans with mental illness are hearing a loud and clear message: Get help. There’s still one question: Who is going to treat them?
The shortage of mental-health providers in the U.S. has long been considered a significant problem. But it is becoming more acute as people are encouraged to seek treatment, or find they are able to afford it for the first time as a result of new federal requirements that guarantee mental-health coverage in insurance plans.
The article comes with a map of the top-10 and bottom-10 states for service provision. The message is clear: Have your breakdown in New England, not the South:
The Guardian:
Funding for mental health services will quadruple as the government prepares to transition service providers to the national disability insurance scheme (NDIS).
The federal government has set aside $1.8bn in the NDIS for mental health services. It currently spends $450m on community care programs, many of which will fall under the NDIS umbrella when the program is fully operational.
The chief executive of Mental Health Australia, Frank Quinlan, said he was “delighted” by the funding allocation, but wanted certainty for a number of programs whose funding is due to expire on 1 July, 12 months before the NDIS will be fully operational.
Too bad we don’t have news like this in the U.K.
Mental health care in Nepal
Conflict and Health:
Globally mental health problems are a serious public health concern. Currently four out of five people with severe mental illness in Low and Middle Income Countries (LMIC) receive no effective treatment. There is an urgent need to address this enormous treatment gap. Changing the focus of specialist mental health workers (psychiatrists and psychologists) from only service delivery to also designing and managing mental health services; building clinical capacity of the primary health care (PHC) workers, and providing supervision and quality assurance of mental health services may help in scaling up mental health services in LMICs. Little is known however, about the mental health policy and services context for these strategies in fragile-state settings, such as Nepal ... Mental health policy exists in Nepal, having been adopted in 1997, but implementation of the policy framework has yet to begin.
Most memorable headline of the week
From The Rakyat Post: Non-married couples on motorcycles will not be arrested, but given counselling.